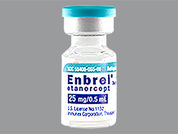
Enbrel
Etanercept
What is Enbrel used for?
This medication is used alone or in combination with an immunosuppressant (such as methotrexate) to treat certain types of arthritis (such as rheumatoid, psoriatic, juvenile idiopathic, and ankylosing spondylitis). Some brands of this medication are also used to treat a skin condition called psoriasis. These conditions are caused by an overactive immune system (autoimmune disease). The immune system attacks the body's own healthy cells, causing inflammation in the joints and skin. Etanercept controls your body's defensive response by blocking the action of a certain natural substance (TNF) that is used by the immune system. Treatment decreases redness, itching and scaly patches in psoriasis as well as the pain, swelling and stiffness of joints in arthritis. This medication can stop the progression of disease and joint damage, resulting in improved daily functioning and quality of life. This medication treats but does not cure autoimmune diseases. Symptoms usually return within 1 month of stopping the medication.
CHEMICAL NAME
DRUG TYPE
Inflammatory ConditionsEnbrel Prices
Searching for the lowest prices
What does Enbrel look like?
View all Enbrel Image Information (4)Enbrel Frequently Asked Questions
Because etanercept works by blocking the immune system, it may lower your ability to fight infections. This may make you more likely to get a serious (rarely fatal) infection (such as fungal infections, bacterial infections including tuberculosis) or make any infection you have worse. Tell your doctor your medical history, especially of past/recent/current infections. Also, tell your doctor if you have lived or traveled in areas where certain fungal infections (such as coccidioidomycosis, histoplasmosis) are common or if you have been near someone with tuberculosis. Areas where these types of fungal infections are commonly found include the Ohio and Mississippi River valleys and the southwestern United States. You should be tested for tuberculosis (TB skin test or chest X-ray) before and during treatment with etanercept. Tell your doctor right away if you have any signs of infection (such as sore throat or cough that doesn't go away, fever, chills, night sweats, painful/frequent urination, unusual vaginal discharge, white patches in the mouth).
The immune system is also important in preventing and controlling cancer. Though it is very unlikely to happen, there is a risk (especially in children/teens/young adults) of developing cancer (such as lymphoma, skin) due to this medication or due to your medical condition. Discuss the risks and benefits of treatment with your doctor. Tell your doctor right away if you develop symptoms such as fever that doesn't go away, unusual lumps/growths, swollen or painful abdomen, unexplained weight loss, or night sweats.
IMPORTANT: HOW TO USE THIS INFORMATION: This is a summary and does NOT have all possible information about this product. This information does not assure that this product is safe, effective, or appropriate for you. This information is not individual medical advice and does not substitute for the advice of your health care professional. Always ask your health care professional for complete information about this product and your specific health needs.